You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Dental veneers have become buzzwords in popular culture; television sitcoms, cinema,and magazine advertising have transformed the professional terminology for these cosmetic techniques into household names. As a result, dental teams are responding to the campaign-driven demands of their patients, becoming highly versed and skilled in placing these metal-free restorations.
|
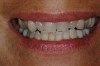
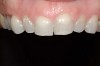
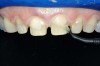
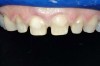
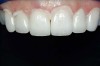
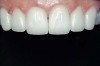
Figure 1 and Figure 2 Preoperative views of a female patient in her mid-50s who presented with a chief complaint of dissatisfaction with the appearance of her smile. Examination revealed multiple fractures, hypocalcification, shortened clinical teeth due to wear, and an asymmetrical smile line. Teeth Nos. 6 through 11 were treatment planned for porcelain laminate veneers. |
The hype surrounding veneers is not vapid or baseless, and beyond their esthetic appeal, these dental restorations are many practitioners' first choice for the treatment of functional dental problems. For example, porcelain veneer restorations can clinically alter and correct faulty occlusal relationships,such as vertical dimension or cuspal guidance.1 Because preservation of tooth structure is important to dentists and patients alike, placing porcelain laminate veneers can be an optimal, conservative alternative to full-coverage crowns, as some researchers have suggested.2,3
In fact, scientists evaluating the long-term functionality of porcelain laminate veneers after 1 to 10 years of service observed that they had been placed for such reasons as correcting fractured and worn anterior teeth, treating surface enamel defects, and changing the appearance of intrinsically discolored dentition (Figure 2');" rem="#ip:figure1 and Figure 2">Figure 1 and Figure 2).2 These researchers found that the porcelain laminate veneer concept provided excellent esthetic and conservative restorations. In other studies, researchers observed 5-year success rates with porcelain laminate veneers,3 commenting that they offer a reliable and effective procedure for the conservative and esthetic treatment of anterior dentition.
The parameters that define long-term success for porcelain laminate veneers encompass functional, clinical, and esthetic aspects of the restorations and their interface with the underlying tooth structure. For example, in aretrospective study of the clinical performance of laminate veneers placed in the anterior segments of dental arches during a 12-year period, the parameters evaluated included the condition of the porcelain surface, marginal discoloration, marginal integrity, and color match.4 Based on the criteria used, most veneers evaluated were rated "A" with the probability of survival of those veneers examined determined to be 94.4% at 12 years, with a low clinical failure rate.4 Significant to this research, however,is the fact that the scientists noted that for porcelain laminate veneers toachieve this survival rate, they must be bonded according to the correctadhesive technique, of which the cementation process is a part.
Other researchers, authors, and educators have made similar observations regarding the importance of cementation and its related processes to the long-term success of veneer restorations based on original research and/or reviews of the literature.5,6 Related processes include tooth preparation, proper material selection (eg, etchants, adhesives, and cements), and proper placement (ie, sufficient application time, use of proper curing instruments at theadequate intensity). Simply stated, an ideal veneer restoration has beenachieved when, among other factors, correct adhesive treatment procedures arecompleted and a suitable luting composite is properly used.6
CAVEATS OF VENEER CEMENTATION PROTOCOL
Therefore,it behooves clinicians and their assistants to help ensure patient satisfaction by avoiding errors during the cementation sequence. The bonding and cementation processes required for placing veneers are essential to making these esthetic restorations functional and comfortable, and the time required differs significantly from that required for conventional restorations.2 Some researchers who have evaluated the long-term service of porcelain laminate veneers have stated that the cementation and finishing processes for these restorations is highly time consuming and requires a greater attention to detail.2
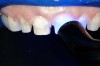
For example, before initiating the cementation process, preparations must be thoroughly cleansed (Figure 3), and adequate hemostasis and isolation should be ensured (Figure 4). Although newer generations of adhesives have been shown to be more tolerant of saliva contamination,7 proper isolation and hemostasis are still advisable because saliva and blood contamination cannegatively influence the bond strength of some bonding systems.8,9 Also,consider that resin cements are preferred for esthetic restorations, including porcelain laminate veneers.10,11 Successful use of these cements is dependent upon the incorporation of proper ceramic conditioning and tooth-surface treatment (ie, multiple-step total etch or self-etch adhesive)(Figure 8');" rem="#ip:figure5 through Figure 8">Figure 5 through Figure 8) to avoid incompatibility issues with the chosen cement and/or enhance the mechanical interlocking that occurs between the porcelain/resin-cement/tooth interfaces.10-13
|
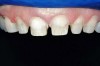
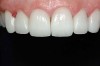
Figure 3 At the cementation appointment, the provisional restorations were removed, and the teeth were thoroughly cleaned. |
|
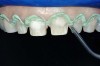
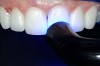
Figure 4 To ensure adequate cervical access and promote hemostasis, a viscous, gingival retraction paste containing aluminum chloride (Expasyl™, Kerr Corporation) was placed in the sulci surrounding the preparations. |
|
Figure 5 A 37.5% phosphoric acid gel (Gel Etchant, Kerr Corporation) was applied to the preparations for 15 seconds, after which they were rinsed and slightly air-dried. |
|
Figure 6 through Figure 8 An adhesive bonding agent (OptiBond® Solo Plus™, Kerr Corporation) was brushed onto the preparations for 15 seconds, per the manufacturer's directions, after which they were air-thinned for 3 seconds and light-cured for 10 seconds. |
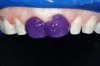
| Figure 9 The clear shade, light-cure version of the selected cement (NX3 Nexus Third Generation) was dispensed directly onto the internal surfaces of the veneer, after which they were placed onto the preparations, allowing excess cement to be expressed from the margins. |
| Figure 10 The restorations were spot-cured for several seconds to allow the excess cement to gel to facilitate clean-up from around the margins. |
|
Figure 11 The veneers were then light-cured for 40 seconds per surface to ensure a complete depth of cure. |
| Figure 12 Occlusion was adjusted using a fine diamond bur, and the lingual aspects of the teeth were finished and polished, rendering a very satisfactory esthetic result. |
| Figure 13 Final postoperative view of the definitively cemented porcelain laminate veneer restorations |
When actually placing the veneers, a cement that demonstrates a low viscosity and a film thickness that facilitates complete seating, yet still provides high strength should be used.14 Film thickness affects proper seating of indirect restorations-particularly veneers-and the industry standard recommends a thickness of 25 m m or less.15
Once the cement has been selected and loaded into the restorations (Figure 9 and Figure10), care must be taken to observe and account for the thickness of the veneers themselves. When light-cured composite cements are used for all-ceramic veneers, the curing time should be increased when activating through porcelain thicknesses of 0.5 mm to 2 mm.16,17 One study in particular suggests that the polymerization of light-cured composite resin luting agents cannot predictably be accomplished through a restoration exceeding 2 mm in thickness if the exposure to the curing light is 90 seconds or less.18 Additionally,curing times may need to be adjusted based on the wavelength of light and the type of light source used (eg, plasma arc light, high-intensity halogen light,conventional halogen light), because light intensities can vary and affect the time necessary to achieve thorough polymerization of the luting cement (Figure11).19-22 With conventional halogen curing units, there may be insufficient light transmission through thicker veneers for adequate light polymerization.22 Also, the curing efficiency of plasma arc light units for curing resin composites under porcelain laminate veneers was shown to be lower compared to the conventional polymerization units tested.21Porcelain opacity, however, has been shown to not have a significant effect on the micro-hardness or bond strengths achieved after polymerization with different types of curing lights.23,24
IMPACT OF CEMENT CHARACTERISTICS ON MICROLEAKAGE AND STRENGTH
The properties and characteristics inherent to the dental luting cements chosen for use in placing porcelain laminate veneers come to bear on the long-term clinical success and overall performance of these restorations. Their composition and performance subsequently affect the microleakage and strength/stress distribution of these esthetic restorations, among other properties.25
The clinical success of cemented restorations is calculated in part by the absence of microleakage, the accuracy of marginal fit, and the subsequent restoration seal.26 Microleakage has been correlated with a decrease in the integrity of the bond to tooth structure in all-ceramic restorations, which can be a catalyst to other problems, such as postoperative sensitivity, pulpal inflammation, secondary caries, tooth staining, and plaque accumulation.27,28The clinically undetectable passage of bacteria, fluids, molecules, or ions between tooth structure and the cemented restoration are to blame for these outcomes.28
Some studies suggest, however, that the occurrence of microleakage with porcelain laminate veneers may be a product of the preparation design and/or the adhesive bonding system used, not necessarily the cement.29,30 When veneers are cemented on dentin margins, bonding agents tested were found to not significantly reduce the marginal leakage of the veneers.29 Also,dentinal exposure is contraindicated because resin bonds better with enamel than with dentin.30
In terms of strength and stress distribution, composite resin cements that are used for placing porcelain laminate veneers are among the cements demonstrating high physical properties, such as high compressive strength, high flexural strength, good fracture toughness, and low coefficient of thermal expansion and contraction, and their inherent properties subsequently affect the properties of the restorations they are used to place.17 The ratio of thickness of cement and luting composite seems to have a relevant influence on stress distribution in porcelain veneers.31 Flowable composite cements can be suitable for cementing porcelain laminate veneers, having demonstrated mean shear bond strengths that are not statistically different from other resin cements.32Resin cements in dual-cure mode have demonstrated higher bond strengths than self-cured materials, but neither may be appropriate for the placement of veneers, as described below.33
CONSIDERATIONS FOR SELECTING TODAY'S RESIN CEMENTS
As previously noted, considering the various factors influencing the cementation process and the ultimate performance of the definitively placed porcelain laminate veneers, resin cements are this author's choice for seating these esthetic restorations. Published researchers such as Strassler and Sensi,17and Kugel,14 among others, have identified desirable characteristics of cements.16,25 These include low viscosity to facilitate seating;ideal film thickness; high strength (eg, shear, tensile, and compressive);being bondable to tooth structure and restorative material; color stability;appropriate shade match; translucency and radiopacity; and easy clean up. The assortment of resin cements available today includes numerous offerings that have been modified and/or specifically formulated to satisfy clinical needs and professional expectations (Table 1).17 Today's resin cements are available as powder-liquid and paste-paste hand-mixing, double-barreled syringe, automixing, and unit-dose dispensing systems.17 They are fairly insoluble, and Strassler and Sensi have noted that because they are based on the composition of direct restorative composites, they demonstrate resistance to wear and abrasion.17
The categories of these resin cements include those requiring the use of separate etchants and bonding adhesives (ie, total-etch), as well as those that are self-etch/self-adhesive.17,34 Strassler and Seni further classify total-etch adhesive resin cements based on their method of polymerization:self-cure (auto-polymerizing), dual-cure (both light- and self-cure), and light-cure only.17 The type of chemical initiators included in the cement formulation determines its polymerization mechanism. However, because self-cure and dual-cure resin cements contain a mine accelerators or initiators,which have a detrimental effect on the long-term color stability of the cement,and light-cure resin cements use a photo-initiator only, it is recommended in the literature that porcelain laminate veneer restorations be placed with light-cure composite resin cements.17,35
Anin vitro study evaluating the color stability of several commercially available resin cements under accelerated conditions found that resin cements tended to change color between 1 week and 14 weeks, with color change values increasing with accelerated aging times.36 A later study involving a self-adhesive resin cement, a resin-based composite cement, a hybrid ionomercement, and a compomer cement revealed that all resin cements evaluated demonstrated perceptible color changes after accelerated aging.37 Dual-cure composite resin cements have also demonstrated both short- and long-term color changes in vitro.38
One manufacturer recently introduced an amine-free self-etch/self-adhesive light-cure resin cement (NX3 Nexus® Third Generation, Kerr Corporation, Orange, CA).According to the manufacturer, this resin cement represents the first truly color-stable adhesive resin cement.39 Testing of the color stability of this amine-free cement showed that its color change was significantly lower after 24 hours than those of other cements evaluated.40 However,more research is needed to substantiate the long-term predictability of its use for the cementation of porcelain laminate veneer restorations.
This recently introduced cement (NX3), among others (eg, RelyX™ Luting Plus Cement,3M ESPE, St. Paul, MN; Variolink®, Ivoclar Vivadent, Amherst,NY ), offers alight-cured modality that provides an expanded window of intraoral working time that is desirable when placing veneers. Another beneficial characteristic of this cement is the incorporation of a simplified, time-saving self-etch bonding system. However, it is important to note that some researchers do not advise the use of self-adhesive resin cements when placing translucent ceramic veneer restorations (eg, pressed ceramic crowns or porcelain veneers) because a color change in the underlying cement could affect the shade of the restoration.17
CONCLUSION
The cementation process for the placement of porcelain laminate veneers is a significant-yet often under appreciated-part of this esthetic restorative process. Understanding the characteristics of the cement selected, as well as the manner in which associated aspects of relevant protocol can impact the predictability of both cement and veneer performance, can greatly enhance the likelihood of realizing clinical success (Figure 13');" rem="#ip:figure12 and Figure 13">Figure 12 and Figure 13). This article has discussed factors that influence cement selection for, and the cementation of, porcelain laminate veneers and why those considerations are significant to the long-term clinical success of these restorations.
REFERENCES
1. Garber DA, Adar P. Securing the position of ceramic veneers in dentistry. Signature. 1997;4:2-4.
2. Dumfahrt H. Porcelain laminate veneers. A retrospective evaluation after 1 to 10 years of service: Part I-Clinical procedure. Int J Prosthodont. 1999;12(6):505-513.
3. Aristidis GA, Dimitra B. Five-year clinical performance of porcelain laminate veneers. Quintessence Int. 2002;33(3):185-189.
4. Fradeani M, Redemagni M, Corrado M. Porcelain laminate veneers: 6- to 12-year clinical evaluation--a retrospective study. Int J Periodontics Restorative Dent. 2005;25(1):9-17.
5. Calamia JR, Calamia CS. Porcelain laminate veneers: reasons for 25 years of success. Dent Clin North Am. 2007;51(2):399-417, ix.
6. Peumans M, Van Meerbeek B, Lambrechts P, Vanherle G. Porcelain veneers: a review of the literature. J Dent. 2000;28(3):163-177.
7. Townsend RD, Dunn WJ. The effect of saliva contamination on enamel and dentin using a self-etching adhesive. J Am Dent Assoc. 2004;135(7):895-901.
8. Park JW, Lee KC. The influence of salivary contamination on shear bond strength of dentin adhesive systems. Oper Dent. 2004;29(4):437-442.
9. Van Schalkwyk JH, Botha FS, van der Vyver PJ, et al. Effect of biological contamination on dentine bond strength of adhesive resins. SADJ. 2003;58(4):143-147.
10. Pegoraro TA, da Silva NR, Carvalho RM. Cements for use in esthetic dentistry. Dent Clin North Am. 2007;51(2):453-471, x.
11. Krämer N, Lohbauer U, Frankenberger R. Adhesive luting of indirect restorations. Am J Dent. 2000;13(Spec No):60D-76D.
12. Addison O, Fleming GJ. The influence of cement lute, thermocycling and surface preparation on the strength of a porcelain laminate veneering material. Dent Mater. 2004;20(3):286-292.
13. Peumans M, Van Meerbeek B, Yoshida Y, et al. Porcelain veneers bonded to tooth structure: an ultra-morphological FE-SEM examination of the adhesive interface. Dent Mater. 1999;15:105-119.
14. Kugel G. Classification and application of cementation alternatives. Signature. 1997;4(3):8-11.
15. Moon PC, Tabassian MS, Culbreath TE. Flow characteristics and film thickness of flowable resin composites. Oper Dent. 2002;27(3):248-253.
16. Powers JM, Sakaguchi RL. Cements. In: Powers JM, Sakaguchi RL, eds. Craig's Restorative Dental Materials. 12th ed. St. Louis, MO: Mosby Elsevier; 2006:480-511.
17. Strassler HE, Sensi LG. Contemporary dental cements to meet the challenges of today's restorative dentistry. Functional Esthetics & Restorative Dentistry. 2007;1(3):44-49.
18. Breeding LC, Dixon DL, Caughman WF. The curing potential of light-activated composite resin luting agents. J Prosthet Dent. 1991;65(4):512-518.
19. Rasetto FH, Driscoll CF, von Fraunhofer JA. Effect of light source and time on the polymerization of resin cement through ceramic veneers. J Prosthodont. 2001;10(3):133-139.
20. Watts DC, Cash AJ. Analysis of optical transmission by 400-500 nm visible light into aesthetic dental biomaterials. J Dent. 1994;22(2):112-117.
21. Usumez A, Ozturk AN, Usumez S, Ozturk B.. The efficiency of different light sources to polymerize resin cement beneath porcelain laminate veneers. J Oral Rehabil. 2004;31(2):160-165.
22. Rasetto FH, Driscoll CF, Prestipino V, et al. Light transmission through all-ceramic dental materials: a pilot study. J Prosthet Dent. 2004;91(5):441-446.
23. Linden JJ, Swift EJ Jr, Boyer DB, Davis BK. Photo-activation of resin cements through porcelain veneers. J Dent Res. 1991;70(2):154-157.
24. Watanabe K, Ohnishi E, Kaneshima T, et al. Porcelain veneer bonding to enamel with plasma-arc light resin curing. Dent Mater J. 2002;21(1):61-68.
25. Rosenstiel SF, Land MF, Crispin BJ. Dental luting agents: A review of the current literature. J Prosthet Dent. 1998;80(3):280-301.
26. Gladys S, Van Meerbeek B, Lambrechts P, Vanherle G. Microleakage of adhesive restorative materials. Am J Dent. 2001;14(3):170-176.
27. Alani AH, Toh CG. Detection of microleakage around dental restorations: a review. Oper Dent. 1997;22(4):173-185.
28. Kidd EA. Microleakage: a review. J Dent. 1976;4(5):199-206.
29. Sim C, Neo J, Chua EK, Tan BY. The effect of dentin bonding agents on the microleakage of porcelain veneers. Dent Mater. 1994;10(4):278-281.
30. Ferrari M, Patroni S, Balleri P. Measurement of enamel thickness in relation to reduction for etched laminate veneers. Int J Periodontics Restorative Dent. 1992;12(5):407-413.
31. Magne P, Versluis A, Douglas WH. Effect of luting composite shrinkage and thermal loads on the stress distribution in porcelain laminate veneers. J Prosthet Dent. 1999;81(3):335-344.
32. Barceleiro Mde O, De Miranda MS, Dias KR, Sekito T Jr. Shear bond strength of porcelain laminate veneer bonded with flowable composite. Oper Dent. 2003;28(4):423-428.
33. Witzel MF, Braga RR, Singer Jde M, Azevedo CL. Bond strength between polymer resin-based cement and porcelain-dentin surfaces: influence of polymerization mode and early cyclic loading. Int J Prosthodont. 2003;16(2):145-149.
34. Platt JA. Resin-based luting cements. Compend Contin Educ Dent. 2000;21(9):740-744.
35. Hekimoglu C, Anil N, Etikan I. Effect of accelerated aging on the color stability of cemented laminate veneers. Int J Prosthodont. 2000;13(1):29-33.
36. Nathanson D, Banasr F. Color stability of resin cements-an in vitro study. Pract Proced Aesthet Dent. 2002;14(6):449-456.
37. Lu H, Powers JM. Color stability of resin cements after accelerated aging. Am J Dent. 2004;17(5):354-358.
38. Berrong JM, Weed RM, Schwartz IS. Color stability of selected dual-cure composite resin cements. J Prosthodont. 1993;2(1):24-27.
39. Manufacturer information. Available at www.kerrdental.com.
40. Nguyen TD, Nguyen TT, Qian X, et al. Color stability of a new dual-cure resin cement. J Dent Res. 2007; In press.
About the Author
Mitch A. Conditt, DDS
Clinical Instructor
Las Vegas Institute
Las Vegas, Nevada
| PRODUCT NAME | MANUFACTURER | MODE OF CURE & ETCH |
| RelyX™ Unicem | 3M ESPE (St. Paul, MN) | Self-Etch/Self-Adhesive |
| RelyX™ Veneer Cement | 3M ESPE (St. Paul, MN) | Light-Cure; Total-Etch |
| BisCem™ | Bisco, Inc (Schaumburg, IL) | Self-Etch/Self-Adhesive |
| Choice™ | Bisco, Inc (Schaumburg, IL) | Total-Etch |
| Choice™ 2 | Bisco, Inc (Schaumburg, IL) | Total-Etch; Light Cure |
| DuoLink™ | Bisco, Inc (Schaumburg, IL) | Total-Etch |
| Illusion™ | Bisco, Inc (Schaumburg, IL) | Total-Etch |
| Duo Cement Plus | Coltene/Whaledent, Inc (Cuyahoga Falls, OH) | Total-Etch |
| ParaCem® | Coltene/Whaledent, Inc (Cuyahoga Falls, OH) | Total-Etch |
| Infinity® Syringeable | Den-Mat Corporation (Santa Maria, CA) | Total-Etch |
| Ultra-Bond® Plus | Den-Mat Corporation (Santa Maria, CA) | Total-Etch |
| Calibra® | DENTSPLY Caulk (Milford, DE) | Dual-Cure; Total-Etch |
| COMSPAN™ | DENTSPLY International (York, PA) | Total-Etch |
| G-Cem™ | GC America, Inc (Alsip, IL) | Self-Etch/Self-Adhesive |
| Twinlook® | Hereaus Kulzer, Inc (Armonk, NY) | Total-Etch |
| Dual® Cement | Ivoclar Vivadent (Amherst, NY) | Total-Etch |
| MultiLink® | Ivoclar Vivadent (Amherst, NY) | Self-Etch/Self-Adhesive |
| Variolink® II | Ivoclar Vivadent (Amherst, NY) | Dual-Cure; Total-Etch |
| Variolink® Veneer | Ivoclar Vivadent (Amherst, NY) | Light-Cure; Total-Etch |
| Maxcem™ | Kerr Corporation (Orange, CA) | Self-Etch/Self-Adhesive |
| Nexus®2™ | Kerr Corporation (Orange, CA) | Dual-Cure; Total-Etch |
| NX3 Nexus® Third Generation | Kerr Corporation (Orange, CA) | Light-Cure or Dual-Cure; Self-Etch or Total-Etch |
| Clearfil® Esthetic Cement & DC Bond Kit | Kuraray America Inc (New York, NY) | Dual-Cure; Self-Etch |
| Panavia F2.0 | Kuraray America, Co (New York, NY) | Dual-Cure; Self-Etch |
| Breeze™ | Pentron Clinical Technologies, LLC (Wallingford, CT) | Self-Etch/Self- Adhesive |
| Lute-It® | Pentron Clinical Technologies, LLC (Wallingford, CT) | Total-Etch |
| Embrace™ WetBond™ | Pulpdent Corporation (Watertown, MA) | Self-Etch/Self-Adhesive |
| ResiLute™ | Pulpdent Corporation (Watertown, MA) | Light-Cure or Self-Cure; Total-Etch |
| MonoCem™ | Shofu Dental Incorporated (San Marcos, CA) | Self-Etch/Self-Adhesive |
| Bistite IIDC | Tokuyama Dental Corp (Encinitas, CA) | Dual-Cure; Self-Etch |
| Tokuyama® M-Bond | Tokuyama Dental Corp (Encinitas, CA) | Self-Cure; Self-Etch |
| PermaFlo® DC Base | Ultradent Products, Inc (South Jordan, UT) | Total-Etch |